No products in the basket.
Blog
Video of a vascular occlusion from dermal fillers
Vascular occlusion video from dermal fillers being injected into an artery.
The most dangerous element of a dermal filler injection is the possibility of injecting into an artery. The tip of the needle is the single most important component to be aware of in terms of position when doing filler injections via either a cannula or a needle. The type of filler you use is not relevant. However, this is based on hyaluronic acid based dermal fillers. BDDE cross linked dermal fillers. They can be from any brand whether it is Juvederm ultra or Vycross. Teosyal or Teoxane. Belotero or Revolax. The brand does not matter. This can happen with any HA based filler. It can lead to necrosis of the tissue and this can leave scarring or even blindness.
Cannula is considered to be safer than needle. However, if a cannula cannulates an artery it can often be more devastating than a needle injury. There are many ways in which you can try to avoid a vascular occlusion. But the single most important thing is to have a comprehensive understanding of an injectors anatomy. We cover this in great detail on our Dermal Fillers Foundation Training course.
Our training course is suitable for medics and non medics alike. Even if you are a fully qualified doctor or nurse you will find our 4 day training course is extremely comprehensive. Our injectors anatomy modules are the finest around.
There are multiple signs a vascular occlusion may have occurred.
- Livedo Reticularis
- Slow capillary refill
There are more but these two are the most significant.
Livedo Reticularis can present itself in the form of mottling. And slow capillary refill can be seen by pressing an area of skin and seeing how long the blood takes to return. If the capillary refill is slow. More than 4-5 seconds. It maybe necessary to seek specialist attention.
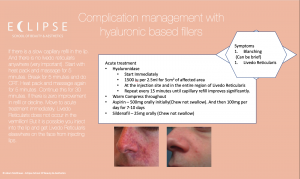
If it is determined that VO is definately present. An emergency protocol should be applied. This can include several items
- Massage
- Heat pack
- Viagra
- Aspirin
- Hyalase – Hyaluronidase (Or equivalent – Disolvidase for example)
In a specific order these can be utilised in order to resolve a vascular occlusion. Dissolving should be the last possible option but it should always be available. In many cases a single vial of hyalase is not enough. One vial is 1500iu. Often many are needed. So we recommend always stocking at least 10. Preferably 20 and all of the appropriate needles and syringes and anything else that maybe required.
You should have a well documented protocol that allows you to fully understand what your steps should be in any given emergency situation. See our diagram below for a comprehensive emergency protocol.
If you have an ultrasound machine this can also be used in order to do vascular mapping of the face in order to be able to build up an accurate understanding of exactly what is going on under the skin and exactly where the vascular occlusion is. Once found it can be easily injected with hyalase and dissolved. We offer specialist ultrasound training with a very high level HD 20Mhz ultrasound scanning device. You can find our training for this here
This ultrasound training for injectors is a very specialist training course and should be for highly experienced aesthetic practitioners. The ability to check depths of arteries and veins and muscles and even facias via ultrasound can be truly revolutionary in regards safe injecting and superior vascular occlusion emergency response.
Even with non BDDE cross-linked products such as profhilo. Sunekos. Jalupro. VO is still possible. If the pressure is significant enough and in the wrong area. And too much product injected. It’s often considered safe. But in the wrong hands it is not safe. Again for these HA based products. Hyalase and your emergency protocol would be important to have to hand.
Botox and other botulinum toxin products such as boccouture and azzalure do not cause vascular occlusion and dissolving of these products is both unnecessary and also impossible. Even with this knowledge it’s very important to have the correct Anti wrinkle injections and botulinum toxin training to make sure the procedure is done correctly and most importantly safely. You can see our training here.
Can PDO threads cause a VO? Or vascular occlusion? PDO threads can also not be dissolved. However if inserted incorrectly could cause damage to blood vessels and again its extremely important that they are administered correctly and safely. Our comprehensive training course covers this In great detail. It can be found here.
Even if a VO is resolved correctly. It’s very important to monitor your client over the coming two weeks and get daily updates via video and photo and phone call. We will always help you through any emergency situation and have significant support in place in case of emergency. 24 hour hotline and multiple support groups across social media.
If you require any assistance we also offer free of charge emergency support to anyone. Even if they did not train with us. Please contact us if you need emergency assistance. We provide this completely free of charge and believe no one should be left to deal with this alone. Whether you be a client or a student practitioner.